EveryVoiceCenter is dedicated to providing patients with a natural body of knowledge regarding holistic health. Our blog will help you understand how to live a more healthy life, and how to use the lab tests that can confirm this. For patients who need help on how to make a real change in their health, or who need help with lab tests results, our blog will give you the answers you need.
A few months ago, I was reading an article at the Huffington Post after seeing the headline “Hair test: do they work?” But I was really confused toward how useful they are, so I decided to start to research about the three tests: strip, serum, and protein. I found out that the strip test is an offshoot of the pregnancy test, the serum test is used in detection of infections, and the protein test detects the food additives.
There has been a lot of research done on the effects of cellphone radiation on the human body. Most of the research is done in laboratories, which can have their limitations. For example, just because the lab tests showed that cell phones are not harmful to humans doesn’t mean they are not harmful in other places. For example, the tests performed in the lab were only done on the blood of the human body. What about the effects of cell phones on the human brain? Or the cells in your body?. Read more about list of lab tests and let us know what you think.
Updated 23. September 2023, medical opinion from
This article outlines the laboratory tests that should be used to monitor your patient’s progress on a low-carb diet. This isn’t a recipe list; rather, it’s a guide to assist you figure out how to best support patients who are starting a low-carb diet.
Keep in mind that many of the typical reference ranges were created for a population eating a high-carbohydrate diet while utilizing this guide. Furthermore, many normal values are affected by the laboratory, gender, patient size, and other factors. We’ll attempt to explain why these measures are so crucial.
Alanine aminotransferase is an enzyme that converts alanine to an amino acid (ALT)

Hepatocellular damage is measured with the ALT test, which is a liver enzyme test. It is frequently increased in metabolic syndrome and obesity, with non-alcoholic fatty liver disease being the most prevalent cause (NAFLD). High amounts may also be caused by excessive alcohol intake and liver diseases such as hepatitis.
When should you check?
Basic understanding is required. Repeat the test every 3 to 6 months if the first result is abnormal.
Ranges of standard reference
10-25 IU/L for women, 10-33 IU/L for men
0,25-0,60 c/l for women 0,25-0,75 c/l for men
Considerations for a low-carb diet

A low-carbohydrate diet generally improves elevated ALT levels caused by metabolic syndrome or NAFLD, at least in the long run.
The first three months after beginning a low-carb diet may see an increase in ALT, which coincides with weight reduction. This rise typically goes away with weight reduction, and ALT levels return to normal.
Boosted level
The following factors may lead to higher-than-normal values:
- Cirrhosis or NAFLD (the most prevalent)
- Drinking a lot of booze
- Medication side effects, such as B. statins, aspirin, and certain sleeping drugs
- Mononucleosis
Extremely high levels may be produced by the following factors:
- Acute viral hepatitis is a kind of hepatitis that is caused by
- overuse of pain relievers like acetaminophen (Tylenol)
- Cancer of the liver
Additional information
ALT is found in serum and many bodily tissues, although it is most closely linked to the liver. It’s typically assessed as part of a diagnostic liver function test to see how well your liver is doing. The most sensitive diagnostics for hepatocellular injury are transaminases (ALT and AST), although they are not particularly specific. Abdominal ultrasonography is suggested for the diagnosis of NAFLD since many individuals with NAFLD have normal ALT levels.
Dextrose in a hurry

Fasting blood glucose (FBG) is a test that is often used to diagnose or evaluate diabetes, monitor hyperglycemia and hypoglycemia, and make treatment choices.
When should you check?
At the very least once a year, at the basic level. Many individuals, on the other hand, find that checking their blood glucose levels many times a day, or even constantly, using a continuous glucose meter, is beneficial (CGM). This gives you real-time data on the impact of your food and other lifestyle decisions on your blood glucose levels.
Ranges of standard reference
Low-carbohydrate diet: 54–100 mg/dL (or more, see below).
3.0 – 5.5 mmol/L for low-carb: 3.8 – 5.5 mmol/L for high-carb: 3.8 – 5.5 mmol/L (or more, see below)
Boosted level
The following factors may lead to higher-than-normal values:
- Type 1 or type 2 diabetes
- Acromegaly
- Pancreatitis, acute or chronic
- Cushing’s syndrome is a condition that affects the adrenal glands.
- Glucocorticoids are one of the drug’s side effects.
- Pheochromocytoma
- Stress
LevelReduction
The following factors may contribute to lower-than-normal values:
- Insufficiency of the adrenal glands
- Consumption of alcohol
- insulin that is produced outside of the body
- Hypopituitarism
- Hypothyroidism
- Insulinoma
- Tumors that are cancerous
- Malnutrition
- Medication side effects, such as B. Oral hypoglycemic medications
- Sepsis
Considerations for a low-carb diet

Patients who eat a low-carbohydrate diet may have lower FBG levels than those who eat according to the conventional food pyramid. The conventional reference ranges reflect a culture that burns carbohydrates rather than fats. When a low-carbohydrate patient enters fat-burning mode and absorbs circulating ketones, their requirement for glucose to sustain normal bodily function may be decreased.
If the patient has been on a low-carbohydrate diet for many months, FBG levels may be regularly between 3.0 and 3.9 mmol/L or 54-70 mg/dL. FBG levels may increase even on a low-carbohydrate diet, which can catch patients and doctors off guard.
The twilight effect is a frequent occurrence that occurs while the muscles are in glucose-deprivation mode, or what some low-carb physicians refer to as adaptive glucose maintenance. Blood sugar levels usually stay low for the remainder of the day, so there’s no need to be concerned. The FBG has the potential to be the day’s greatest value.
A1c haemoglobin (HbA1c)
By measuring the amount of glucose molecules attached to red blood cells, hemoglobin A1c (HBA1c) predicts the average blood glucose level during the previous three months. Glycated hemoglobin, also known as glycosylated hemoglobin, is a kind of hemoglobin that contains glucose molecules.
When should you check?
Basic understanding is required. If there is a problem, the procedure should be repeated every three months.
Ranges of standard reference
Typical readings range from 4% to 6%.
5.7% to 6.4% of people have pre-diabetes.
6.5 percent of people have diabetes.
Values that are too high
The following factors may lead to higher-than-normal values:
- Diabetes is a disease that affects people (type 1 and 2)
- Prediabetes
- Low red blood cell (RBC) turnover, e.g. B. Anemia due to iron deficiency
- Deficiency in B12 and folic acid
Values are decreasing.
The following factors may contribute to lower-than-normal values:
- For example, a high proportion of erythrocytes. Hemolytic anemia (B)
- Abuse or misuse of erythropoietin (EPO)
- Treatment for anemia, B12 insufficiency, or folic acid deficiency
- Patients who are on dialysis (which alters the renewal of erythrocytes).
Considerations for a low-carb diet

Prescribe a HbA1c test every three months to encourage patients to stick to their low-carbohydrate diet. When levels drop, individuals get positive incentives; when levels increase, they may be more motivated to stick to a low-carb diet.
The higher rates of previously successful patients returning to their former eating patterns may encourage them to do so. HbA1c readings may plateau or even increase in some individuals when they begin a low-carb diet, particularly when diabetic medication is taken down. Let them know it’s all right.
Example: A patient’s HbA1c is 7.4% at baseline, but he or she is taking 100 units of long-acting insulin per day, a high-dose sulfonylurea derivative, and an SGLT2 inhibitor. Within six months of adhering to a low-carb diet, the patient was able to discontinue using all of his diabetic medicines. After six months, the HbA1c level is still 7.4%. Despite her best efforts, the patient’s HbA1c level does not decrease, leaving her angry and perplexed.
In low-carb clinics, this is a frequent occurrence. However, you may assist the patient in recognizing that it is an improvement! Previously, they needed more insulin and three extra medicines to manage their diabetes; today, they don’t require any medications to maintain the same HbA1c level. This is most likely a sign of increasing insulin sensitivity, which should improve with time. This concept will be reinforced if you revisit it on a regular basis.
Additional information
In individuals with chronic kidney disease (CKD), HbA1c values may be incorrect, underestimating real blood glucose levels. For some genetic variations of hemoglobin, such as fetal hemoglobin (HbF) retention, sickle cell anemia, or if the measurement is excessively high or too low relative to the real blood glucose level, the findings may be incorrect.
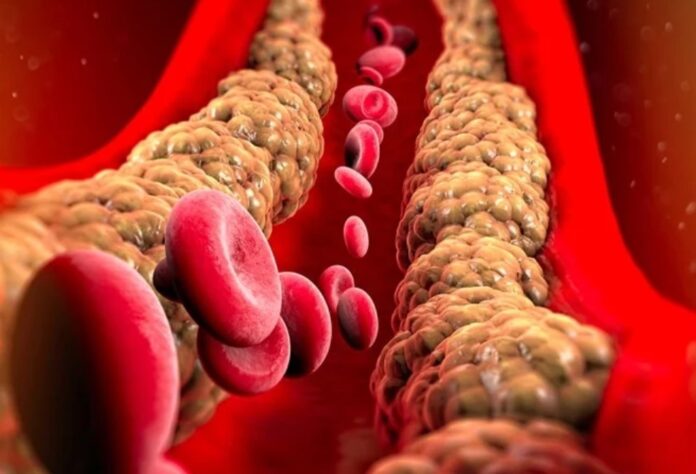
Panel of lipids in their entirety
Cholesterol total, high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), and triglycerides are all measured in the full lipid panel. It’s mostly utilized to determine cardiac risk and therapy options for high-risk individuals.
When should you check?
Basic understanding is required. Every six months, repeat the process. If the patient is hyperreactive, which means that a low-carb diet causes LDL-C to rise substantially, the diet should be repeated every three months until stability is reached, then every six months.
- Ranges of standard reference
- Total cholesterol
- HDL-C
- >40 mg/dl for men and >50 mg/dl for women
- LDL-C
<100 mg/dL (however, it is difficult to give an exact number that is high because LDL levels should be considered as part of the overall risk of CVD and therefore the number of points of concern may vary from person to person)
Triglycerides
Considerations for a low-carb diet
Patients should fast for 12 hours prior to laboratory testing to obtain a complete lipid profile, as diet can cause significant fluctuations in triglyceride levels. It should be noted that the normal values were probably established in people on a high carbohydrate diet. Most patients who follow a low-carb diet have significantly lower triglyceride levels.
Therefore, physicians following a low-carb diet believe that the optimal triglyceride level for patients following a low-carb diet should be lower than 100 mg/dL and closer to 70 mg/dL (<0.8 mmol/L). Most studies indicate that people on a low-carbohydrate diet had lower TG levels and greater HDL levels than those on a high-carbohydrate diet.
During active weight reduction, however, some individuals may have an initial increase in LDL levels, which typically normalizes during the first six to twelve months. When choosing whether or not to take action, it’s essential to keep this connection with weight reduction in mind.
LDL cholesterol levels may increase substantially in approximately 5-25 percent of individuals, with or without weight reduction, in response to a low-carbohydrate diet, occasionally by 200 percent or more. Many of these individuals are members of the Hyperponder Lean Body Masses, as described by Dave Feldman of Cholesterol Code (LMHR).
These usually healthy individuals are frequently surprised to see that after starting the keto diet, their LDL cholesterol has risen by more than 200 mg/dL (5.2 mmol/L). Because there is a scarcity of scientific data on this group of individuals, each case must be assessed on its own merits. Check out our recommendations on low-carb diets and cholesterol, our stance on LDL cholesterol, and how to reduce your LDL with a low-carb diet for additional information.
Creatinine
The measurement of creatinine is a clinical indicator of renal function. The amount of creatinine in the blood is determined by the patient’s muscle mass, age, gender, and glomerular filtration rate (GFR). As a result, depending on these factors, the typical reference ranges may also differ.
When should you check?
Basic understanding is required. If the findings are abnormal or you suspect the patient has CKD, repeat the test every 6 months.
Ranges of standard reference
0.8-1.4 milligrams per deciliter (remember that the normal range varies with gender, age and amount of muscle mass)
Values that are too high
The following factors may lead to higher-than-normal values:
- Acute tubular necrosis is a condition in which the tubules of the body is a condition in which the tubules of the body
- Aminoglycoside antibiotics, for example, have side effects.
- Heart failure due to congestive heart failure
- Dehydration
- Diabetic nephropathy is a kidney disease caused by diabetes. is a kidney disease caused by diabetes.
- Glomerulonephritis
- Failure of the kidneys
- Hypothyroidism
- Muscular dystrophy is a kind of muscular dystrophy. is a kind of muscular dystrophy.
- Pyelonephritis
- Rhabdomyolysis
- Shock
- blockage of the urinary tract
Values are decreasing.
The following factors may contribute to lower-than-normal values:
- Muscle mass reduction
- myasthenia gravis is a disease that affects the muscles.
- Muscular dystrophy
Considerations for a low-carb diet
In the first few weeks or months after starting a low-carb diet, patients shed extra water weight. Doctors may notice a small rise in creatinine levels after a low-carb diet. After 2 to 3 months on a low-carb diet, these levels return to normal.
Some individuals worry that a low-carb or ketogenic diet may harm their kidneys. This is, however, a misconception that is not backed up by scientific data. In our guide to low-carb diets and renal health, we go into this subject in depth.
Urine microalbumin/creatinine ratio
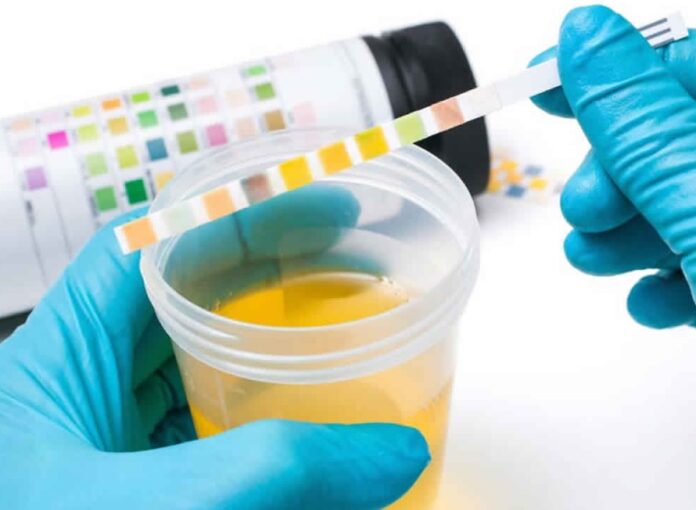
The microalbumin/creatinine ratio (urine) is a frequent diagnostic for early diabetic nephropathy diagnosis. This test, also known as microalbumin, ACR, UACR, or urine albumin, examines how much albumin is released into the urine by the kidneys.
Microalbuminuria may be detected by collecting 24 hours of urine or by a high concentration in a spot urine sample. In at least two of the three measurements, these two indicators should be assessed within two to three months.
When should you check?
Basic understanding is required. Repeat the test every 6 months if the results are abnormal or if the patient has CKD. Repeat the procedure every year after the numbers have stabilized.
Ranges of standard reference
A result of less than 30 mg/dL is considered normal, whereas a range of 30 to 300 mg/dL may suggest early renal disease.
Values that are too high
The following factors may lead to higher-than-normal values:
- Chronic kidney disease is a condition that affects the kidneys (CKD)
- Heart and circulatory problems
- Type 1 or type 2 diabetes
- Diabetic nephropathy
- Blood pressure that is too high
- Endothelial dysfunction in the arteries
Low-carbohydrate diet guidelines
Although there is no proof that a low-carbohydrate diet improves the albumin/creatinine ratio, anecdotal experience and published case reports indicate that this is the case. Low-carb diets, on the other hand, are unlikely to impact renal function, as we explain in our low-carb diets and kidney function guide.
Blood tests that aren’t required
Depending on your patients’ other medical problems, such as. You may request further tests if you have chronic renal illness or hypothyroidism, for example. When patients transition to a low-carbohydrate diet, they may have induction or keto fever. Some tests, such as B. for salt and B. for vitamin B12, may help rule out other possible causes of the symptoms.
a full blood count (CBC)
The amount of red blood cells, white blood cells, and platelets in the blood is determined by a complete blood count (CBC). Platelets (thrombocytes) help blood clot and red blood cells (erythrocytes) provide oxygen. White blood cells are the cells that make up the blood. (leukocytes) form part of the immune system. Red blood cells have a lifespan of 120 days, or three months. As a result, the HbA1c level is checked at least once every three months.
When should you check?
If your patient is fatigued, pale, or has bleeding issues, call 911 immediately.
Ranges of standard reference
White blood cells
The Royal Bank of Canada (RBC) (red blood cell count)
Females: 4–5 million cells per liter 5 million-6 million cells/L in men
Hbg vs. Hb (haemoglobin)
12-15 gm/dl for women 14-17 gm/dl for men
htt (haematocrit)
36 percent to 44 percent of women Men make about 41% to 50% of the population.
MCVVVVVVVVVV (mean corpuscular volume)
Plates
140,000–450,000 cells per liter
Values that are too high
The following factors may lead to higher-than-normal values:
- Heart abnormalities that are present at birth
- Dehydration
- Exceptional height
- Hypoxia is a condition in which there is (e.g. from undiagnosed sleep apnea)
- Tumors that are cancerous
- polycythemia vera is a kind of polycythemia.
- Fibrosis of the lungs
- Thalassemia
Values are decreasing.
The following factors may contribute to lower-than-normal values:
- Anaemia
- Renal failure that has been present for a long time
- Addiction to Alcohol
- B. Allopurinol is an example of a drug that has a side effect.
- Irritable Bowel Syndrome (IBS)
Considerations for a low-carb diet
If your patient is experiencing unexplained tiredness or mental illness, a CBC test may be beneficial. These symptoms may also occur if a patient’s protein, calorie, or salt intake is inadequate, or if they have induction flu or keto flu.
Electrolytes are a kind of ion (sodium and potassium)
Sodium
When following a low-carb diet, monitoring your salt levels may help you avoid symptoms like tiredness, muscular cramps, and headaches. Sodium is an electrolyte that aids in the regulation of blood volume, blood pressure, water balance, nerve induction, muscular contraction, osmotic balance, and acid-base balance, among other things.
When should you check?
Basic understanding is required. In individuals with CKD, repeat every 6 months.
Ranges of standard reference
Values that are too high
The following factors may lead to higher-than-normal values:
- Cushing’s disease/syndrome
- Dehydration
- Excess sodium consumption in the diet
- Type 1 or type 2 diabetes
- diabetes insipidus (diabetes insipidus) is
- Diaphoresis that is excessive
- Age
- Hyperaldosteronism
- Oral contraceptive pills are a kind of contraception that is taken orally.
- Vomit
Values are decreasing.
The following factors may contribute to lower-than-normal values:
- ACE inhibitors and thiazide diuretics are examples of medication side effects.
- Acute tubular necrosis
- Insufficiency of the adrenal glands
- Heart failure due to congestive heart failure
- Cirrhosis
- Diarrhea
- Excessive physical exercise is harmful to your health.
- Sweating excessively
- Hypothyroidism
- Malnutrition
- Nephrotic syndrome is a condition that affects the kidneys.
- Syndrome of antidiuretic hormone deficiency (ADHS)
- Vomit
- Intoxication by water
- Insufficient sodium in the diet
Considerations for a low-carb diet
When moving to a low-carb diet, healthy individuals and even those with renal failure, notwithstanding CKD, may need to increase salt. Patients who quit eating processed meals high in salt lose weight and have reduced water retention. Patients with CKD who follow a low-carbohydrate diet typically have salt levels that stay in the lower half of the normal reference range, but decrease to the point where they suffer moderate hyponatremia symptoms including headache, disorientation, muscular cramps, weakness, and tiredness.
Potassium
Muscle cramps, tiredness, and other symptoms may be alleviated by controlling potassium levels (K+). Potassium is an electrolyte that plays a role in muscular contraction, nerve transmission, heart rhythm, and acid-base balance, among other things.
When should you check?
Basic understanding is required. In individuals with CKD, repeat every 6 months.
Ranges of standard reference
3.6-5.0 mEq/L in American units 3.6-5.0 mmol/L in SI units
Values that are too high
The following factors may lead to higher-than-normal values:
- ACE inhibitors, angiotensin receptor blockers (ARBs), beta blockers, spironolactone, and nonsteroidal anti-inflammatory drugs (NSAIDs) all have side effects.
- Acidosis
- Renal failure, acute or chronic
- Addison’s disease is a condition that affects the adrenal glands.
- Dehydration
- Type 1 and type 2 diabetes are two types of diabetes.
- Infection
- Tissue injury that is severe
- Hemolysis en masse
- Acidosis of the tubules of the kidneys
Values are decreasing.
The following factors may contribute to lower-than-normal values:
- Ascites
- Burns
- Pyelonephritis (chronic pyelonephritis)
- Cushing’s syndrome is a condition that affects the adrenal glands.
- Drug side effects, such as B. diuretics, salicylates, extended corticosteroid therapy, and exogenous insulin
- Diarrhea
- Bulimia and/or laxative abuse are examples of eating disorders.
- Hyperaldosteronism
- Hypothyroidism
- potassium deficiency
- Alkalosis metabolique
- Acidosis of the tubules of the kidneys
- Vomit
Considerations for a low-carb diet
Potassium supplementation is usually unnecessary for most people on a low-carb diet. Check to determine if medicines like blood pressure medication may be changed if your patient is more hyperkalemic. If they can’t, tell them to avoid foods high in potassium, such as avocados, mushrooms, and spinach.
c-peptide or rapid insulin
Fasting insulin or c-peptide tests may provide information about a patient’s insulin production, sensitivity, or resistance to insulin. Although the variability of c-peptide may be lower than that of insulin when tested sober, the two tests offer comparable information, thus it is unlikely that both tests are required.
Both tests measure the amount of insulin produced and used by the body, which is produced by the islets of Langerhans in the pancreas. Insulin is a hormone that regulates carbohydrate and fat metabolism in the body, ensuring that cells in the liver, muscles, and adipose tissue receive glucose from the bloodstream. Diabetes type 2 is caused by insulin resistance.
The HOMA-IR may be calculated using the fasting insulin level and fasting blood glucose, which provides a reasonably good assessment of the metabolic syndrome and is probably better than fasting blood glucose or HbA1c alone.
Traditionally, the c-peptide test has been used to distinguish between type 1 and type 2 diabetes. However, as demonstrated above, it may assist identify insulin resistance long before the development of type 2 diabetes.
When should you check?
Every six months and at the baseline
Ranges of standard reference
Insulin has a short half-life: 2-12 mIU/ml. It’s worth noting that this test for evaluating metabolic health is still quite new, and a precise reference range has yet to be defined. Fasting C-peptide content: 0,78-1,89 mg/ml
Insulin level in the fasting state: 12-72 pmol/l c-peptide level at fasting: 0.26-0.62 nmol/l
Fasting insulin levels are higher.
The following factors may lead to higher-than-normal values:
- Acromegaly
- Cushing’s syndrome is a condition that affects the adrenal glands.
- Diabetes type 2
- Drug side effects, such as B. glucocorticoids, hypoglycemics, and insulin (exogenous)
- Irritable Bowel Syndrome (IBS)
- Insulinoma
- Obesity
- Uremia
Fast insulin levels have dropped.
The following factors may contribute to lower-than-normal values:
- Chronic pancreatitis is a disease that affects the pancreas.
- Kind 1 diabetes is a type of diabetes in which the body
- Hypopituitarism.
C-peptide levels have risen.
The following factors may lead to higher-than-normal values:
- Type 2 diabetes
- Insulinoma
- Failure of the kidneys
C-peptide levels are dropping.
The following factors may contribute to lower-than-normal values:
- Kind 1 diabetes is a type of diabetes in which the body
- Pancreatectomy (complete removal of the pancreas)
- Adults with diabetes of unknown etiology (LADA)
Low-carbohydrate diet guidelines
Stress, illness, lack of sleep, and a recent carbohydrate-rich meal may all affect insulin and c-peptide levels. Patients may be frustrated by significant short-term changes. Regularly reviewing these numbers may assist uncover patterns that can be used to evaluate the success (or lack thereof) of dietary treatments.
Rapid insulin or c-peptide levels typically drop after a low-carbohydrate patient has grown acclimated to fat.
Rapid low-carbohydrate insulin reference periods
0,3 – 5,8 mIU/ml in American units 2 – 40 pmol/L in SI units
Many low-carb dieters aim for a value of 0.3 to 2.9 mIU/ml.
Reference ranges for fasting C-peptide at low carbohydrate levels
0,39 – 1,98 mg/mL in SI units 0.13 – 0.62 nmol/L in SI units
This is a typical range for individuals who have a minimal carbohydrate consumption, but if they eat carbs, these levels may signal the beginning of type 1 diabetes or late-onset type 1 diabetes (LADA). In low-carbohydrate individuals with low insulin or c-peptide levels but rising blood glucose, LADA should be explored.
C-reactive protein (CRP) is a highly sensitive protein (hs-CRP)
As an inflammatory marker, the high-sensitivity c-reactive protein (hs-CRP) test is employed. CRP levels may be measured and recorded to assist assess disease progression and therapy efficacy. It may be an indication that your body is responding to anything in your food (such gluten or processed carbs) or something in your body (like an infection or chronic inflammation).
CRP is produced by the liver as part of the immune system, and it attaches to dead or dying cells to signal phagocytes to remove them.
When should you check?
Basic understanding is required. For individuals with inflammatory disorders or those who experiment a lot with their food, repeat every 3 to 6 months.
Ranges of standard reference
<3 mg/l
Values that are too high
The following factors may lead to higher-than-normal values:
- Atherosclerosis
- Rheumatoid Arthritis (RA) is a kind of arthritis that affects the joints.
- Autoimmune illness is a kind of autoimmune disease.
- Infections
- Diseases of Inflammation
- Tumors that are cancerous
Considerations for a low-carb diet
CRP levels are often lower in patients who follow a low-carbohydrate diet, indicating that they are experiencing less inflammation and encouraging them to continue with this lifestyle. Inflammatory symptoms such as joint pain and edema may often be alleviated.
Nuclear magnetic resonance (NMR) lip profile (NMR)
Lipoprofile or particle analysis using nuclear magnetic resonance imaging (NMR) is a more comprehensive examination of circulating cholesterol that may assist assess a patient’s risk of cardiovascular disease. This test may be especially helpful for determining the quantity and size of low-density lipoprotein (LDL) particles.
When should you check?
Initially, and then every year, or sooner if there are substantial dietary changes.
Considerations for a low-carb diet
This test isn’t commonly accessible, and it’s possible that it won’t be reimbursed by your insurance. Low-carbohydrate diets are usually successful in lowering small LDL while raising overall LDL. This test may be helpful for hyperresponders, or individuals with high LDL levels, to see whether the percentage of bigger, less dense particles has risen rather than the proportion of smaller, more essential particles.
Hormone that stimulates the thyroid (TSH)
Thyroid stimulating hormone testing can tell you if your thyroid is underactive or hyperactive. TSH, which is produced by the pituitary gland and instructs the thyroid how much T3 and T4 it should make, is measured in the blood. TTH levels that are abnormal aren’t necessarily indicative of hypo- or hyperthyroidism. TSH level interpretation is further influenced by T3 and T4 blood levels, clinical indications of thyroid illness, and physical examination.
When should you check?
If the patient has a history of hypothyroidism or Hashimoto’s illness (Hashimoto’s thyroiditis) is a, or is on thyroid medication, this is the starting point. Repeat every three months until the readings have stabilized, then once a year.
Ranges of standard reference
Values that are too high
The following factors may lead to higher-than-normal values:
- Hypothyroidism
- Hashimoto’s disease
- Following an acute sickness, there is a period of recovery.
Values are decreasing.
The following factors may contribute to lower-than-normal values:
- A medical or surgical emergency
- Graves’ disease is a chronic illness that affects people.
- Hyperthyroidism
- Addiction treatment using glucocorticoids or somatostatin analogues, for example.
Considerations for a low-carb diet
Thyroid function may improve somewhat or substantially in individuals with pre-existing hypothyroidism or Hashimoto’s disease when they follow a low-carbohydrate diet. Some physicians who follow a low-carb diet have even been able to get their hypothyroidism patients to quit using medication.
Other people may need to decrease their thyroid medication if they develop hyperthyroidism symptoms, which may appear in waves over many months if they follow a low-carbohydrate diet. As long as the patient is suffering hyperthyroidism symptoms, a low-carbohydrate diet should not be stopped. Some doctors advise against fasting until the patient is on a steady drug dosage.
Hypothyroidism causes fatigue, which is a frequent symptom. It’s easy to mix it up with calorie deficiency, protein deficiency, induction, and the keto flu. TSH testing may assist you figure out why your patient is having these problems.
Uric acid
A uric acid test is performed to determine whether or not a patient has metabolic syndrome. Purine breakdown product detected in the urine. Uric acid levels are a risk factor for diabetes on their own. Gout and kidney stones are both caused by too much uric acid in the body. These figures may be influenced by factors such as diet, alcohol intake, and renal function.
When should you check?
Basic understanding is required. Patients with a history of gout should repeat the test every 6 months.
Ranges of standard reference
4.0 to 8.0 milligrams per deciliter (although the normal range for women may be slightly lower than for men)
Considerations for a low-carb diet
When patients start a low-carb diet, their uric acid levels may temporarily rise. This may be seen in the first six weeks, when patients enter a fat-burning condition before returning to normal.
Patients with a history of gout may be more likely to develop gout again in the first six weeks after switching to a low-carbohydrate diet, although there is no evidence to support this. Patients at risk for gout should be informed about the benefits and drawbacks of preventative therapy.
B12 (cobalamin)
Vitamin B12 (cobalamin) levels may assist diagnose tiredness and other symptoms that might be caused by a poor diet, malabsorption, or malnutrition. Vitamin B12 is a water-soluble vitamin that is essential for brain and nervous system function as well as red blood cell production. Every cell in the human body uses it for a variety of functions, including DNA synthesis and control, fatty acid synthesis, and energy generation.
When should you check?
Vegetarians and vegans, as well as patients who have had gastric bypass surgery or gastric banding in the past, should start here. If there is a problem, the procedure should be repeated every 6 months.
Ranges of standard reference
Reference ranges range from 180 to 900 ng/L (notice that reference intervals differ per laboratory). The Mayo Clinic’s standard laboratory is the source of this information.
Values are decreasing.
The following factors may contribute to lower-than-normal values:
- Resection of the small intestine (gastric bypass, gastrectomy)
- Celiac illness is a kind of celiac disease that
- Crohn’s disease is a chronic inflammatory bowel illness that affects
- Deficiencies in nutrition (veganism)
- An infection of helminths
- Hyperthyroidism
- Malabsorption
- Medication side effects, such as B. Metformin with oral contraceptive pills
- Pernicious anemia is a kind of anemia that is caused by
- Pregnancy
Low-carbohydrate diet guidelines
B12 levels should be sufficient if you eat a low-carbohydrate, high-animal-products diet. It should be mentioned that if a patient has macrocytic anemia due to B12 deficiency, the HbA1c test result may be incorrect (elevated). Fatigue and brain fog are two of the most frequent symptoms of vitamin B12 insufficiency, which may be misinterpreted for insufficient protein and calorie intake, induction, or keto flu. Vitamin B12 levels may assist you figure out why your patient is experiencing these symptoms.
Additional information
Returning to doctors’ main low-carb diet recommendations.
We are often told that a healthy diet consists of fresh fruits and vegetables, whole grains, low fat foods, and limited protein, but until recently, healthy diets were more myth than fact. Underlying all of the hype of over-hyped “healthy diets” were real concerns about what exactly was in the food we were eating. At the center of the debate was the public’s increasing interest in facts.. Read more about clinical laboratory tests and let us know what you think.
Frequently Asked Questions
What are common lab tests?
Common lab tests are blood, urine, and stool.
What are the 5 blood tests?
The 5 blood tests are as follows: 1. Complete Blood Count (CBC) 2. Chemistry Panel 3. Thyroid Function Test 4. Urinalysis 5. Lipid Profile
What are routine lab tests?
A routine lab test is a type of medical test that is done to check for signs of disease or other health problems.